Hysterectomy
9 Nov 2018 | 6 min Read
Babychakra
Author | 1369 Articles
What is hysterectomy?
The surgical removal of the uterus is called hysterectomy. There are multiple conditions for which hysterectomy may be advised. A total, partial, or radical hysterectomy may be performed based on the disease condition.
When is a hysterectomy recommended?
A hysterectomy is advised for various health conditions such as:
- Uterine fibroids: These are noncancerous growths in the uterus that cause back and leg pain, heavy bleeding during menses, longer periods, increased urination, and constipation, for which a hysterectomy is commonly advised.
- Chronic pain in the pelvis: Hysterectomy is an approved treatment method for this condition.
- Ovarian, cervical, and uterine cancers.
- Uterine thickening, also called adenomyosis.
- Endometriosis, the abnormal growth of the tissue lining the uterus.
- Uterine prolapse, a condition where the uterus collapses into the vaginal canal.
- Abnormal and heavy bleeding from the vagina.
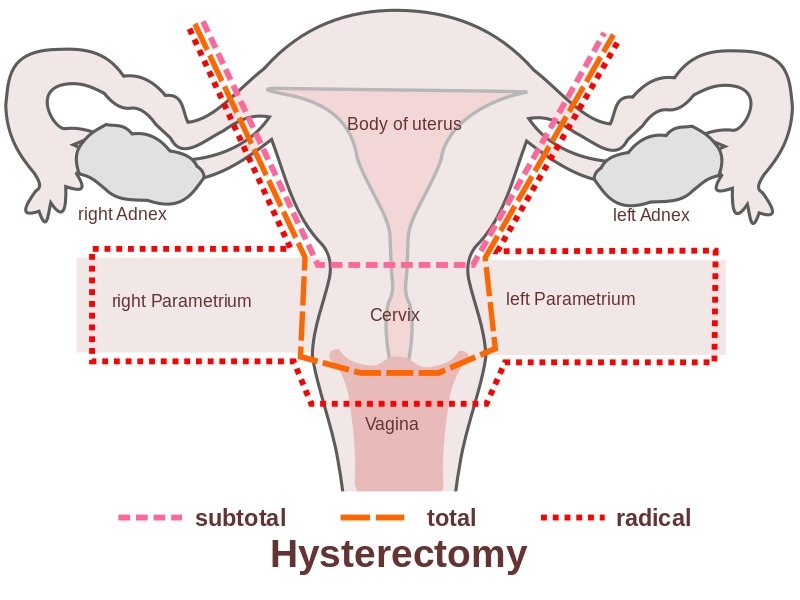
Types of hysterectomy
- Depending on which organs are removed, different types of hysterectomy are performed.
- Total hysterectomy: As the name indicates, the uterus along with the cervix is removed.
- Partial hysterectomy: Also called supracervical or subtotal hysterectomy, only the uterus is removed, not the cervix.
- Radical hysterectomy: A total hysterectomy, this procedure entails removal of the cervix, uterus, and the surrounding tissues and structures. This type of hysterectomy is preferred in patients with cancer.
- An oophorectomy (removal of ovaries) and salpingectomy (removal of the tubes that carry the eggs from the ovaries to the uterus) may also be advised as needed.
Pre-surgery care
Before beginning the operation, the doctor will:
- Conduct tests to make sure the patient will be able to tolerate surgery
- Perform a complete physical examination
- Ask the patient to discontinue smoking a few weeks before the surgery if they smoke
- Make sure medical conditions such as high blood pressure, diabetes, lung or heart problems, are under adequate control before the surgery
- Advise the patient to stop taking blood-thinning medications temporarily
To prevent any complications, the doctor should be informed of:
- Any prescribed and non-prescribed supplements, herbs, vitamins, or medications
- Any allergies
- Alcohol intake of more than one to two drinks in a day
- The possibility of a pregnancy
Precautions on the day of surgery:
- Arrive at the hospital on time for surgery
- Avoid eating and drinking from midnight prior to the surgery unless instructed
- Follow the instructions given by the doctor for bowel preparation prior to the surgery
- Take the pre-surgery medications with small sips of water
The hysterectomy procedure
The hysterectomy approach depends upon the condition that is being treated.
Open surgery: Also called an abdominal hysterectomy, the uterus is removed through an incision in the abdomen. An incision of five to seven inches in the lower abdomen gives a clear view of the abdominal structures and allows removal of the uterus. Open surgery will leave a scar on the abdomen.
Minimally invasive procedure: These procedures require minimal surgical incisions, thus facilitating faster recovery and reduced pain.
Types of minimally invasive procedures:
- Vaginal hysterectomy: The uterus is removed through the vagina without the need for an abdominal incision. This procedure cannot be performed in certain conditions such as a large uterus.
- Laparoscopic hysterectomy: This method involves a few small incisions in the abdomen. The laparoscope is inserted through one incision to view the pelvic organs. The uterus is removed either through the small incisions, through the vagina (laparoscopic vaginal hysterectomy), or through a larger incision in the abdomen.
- Laparoscopic vaginal hysterectomy: This method involves the removal of the uterus through the vagina with the assistance of a laparoscope.
Robot-assisted laparoscopic hysterectomy: In this method, the surgical instrument (robotic) for hysterectomy is controlled by a surgeon using a computer.
Post-surgery care
- A post-procedure hospital stay of one to two days or more is required to monitor the following:
- Blood pressure, pulse rate, breathing pattern and the wound will be monitored.
- A urinary catheter may be inserted to drain urine.
- Intravenous fluids (fluids directly delivered to the vein) will be administered.
- Medications will be provided to ease the pain.
- Wound care will be provided, and the patient will be kept under observation.
- The patient will be asked to walk at the earliest after the surgery to lower the risk of chest infection and blood clots.
- Medications and instructions for wound care at home will be given at discharge.
A follow-up appointment will be set.
Post-surgery care at home
The following are some do’s and don’ts when you are home after your hysterectomy:
Do’s
- You should slowly start routine activities at about four to six weeks after hysterectomy
- Walk often but slower than your usual pace
- Begin gentle exercises at four to six weeks to reduce the risk of blood clots in the veins of your legs and perform the exercises prescribed by your physiotherapist
- Follow a healthy and balanced diet to accelerate your healing process, include fresh fruits and vegetables, fiber-rich, protein-rich foods and plenty of liquids in your diet
- Wound care: If you have undergone an open hysterectomy or laparoscopic hysterectomy, you may have an incisional wound to take care of. Bathe or shower daily to prevent infection. Change the wound dressing daily or as advised by the doctor
- Use medications as per your doctor’s instructions
Don’ts
- Do not pull, push, or lift heavy objects.
- Do not bend and/or stay longer in the bent position.
- Avoid heavy household chores
- Avoid sexual intercourse for a duration of four to six weeks
- Do not exercise vigorously
In most cases, hysterectomy relieves you from the health condition for which this procedure was performed. If you feel depressed due to thoughts of not being able to conceive a child, you can consult your doctor.
Complications
- Hysterectomy is major surgery and comes with a list of risks and complications. The risks and complications may vary depending on the type of hysterectomy performed.
- Vaginal hysterectomy: The complications in vaginal hysterectomy are minor compared to the other two methods. It is considered the first choice for hysterectomy.
Abdominal hysterectomy: Due to a larger incision, there is a higher risk of tissue and nerve damage, bleeding, infection in the wound, and blood clot seen with abdominal hysterectomy. - Laparoscopic hysterectomy: The laparoscopic hysterectomy procedure may take a longer time than the other two methods. It also has a high risk of damaging the surrounding organs and tissues such as the urinary tract and other organs.
The possible complications of hysterectomy irrespective of the method used are:
- The inability to control urination
- Vaginal prolapse
- Chronic pain
- Blood clot
- Infections and/or damage to the surrounding tissues
- Abnormal growth between the bladder and the vagina
- Hemorrhage
The doctor should be contacted immediately if any of the following symptoms are seen after surgery:
- Chills
- Excessive vaginal bleeding
- Fever
- Chest pain or breathlessness
- Problems in urination and bowel movement
Reference
https://www.mayoclinic.org/diseases-conditions/uterine-fibroids/symptoms-causes/syc-20354288
https://www.ncbi.nlm.nih.gov/pubmed/21508759
https://www.acog.org/Patients/FAQs/Hysterectomy
https://www.nhprovidenceobgyn.org/patient-tools/pre-op–post-op-instructions.aspx
https://www.hopkinsmedicine.org/healthlibrary/test_procedures/gynecology/robotic_hysterectomy_135,12
A


Related Topics for you
Suggestions offered by doctors on BabyChakra are of advisory nature i.e., for educational and informational purposes only. Content posted on, created for, or compiled by BabyChakra is not intended or designed to replace your doctor's independent judgment about any symptom, condition, or the appropriateness or risks of a procedure or treatment for a given person.
